Erysipelas – Bacterial Skin Infection
Comprehensive guide on erysipelas infection.
Introduction
Erysipelas is a bacterial skin infection characterized by painful, red, and swollen areas on the skin. It is a type of cellulitis that affects the upper layers of the skin and is usually caused by Streptococcus bacteria. Understanding erysipelas requires knowledge of its symptoms, causes, and the ways it can be effectively treated. This article aims to provide a comprehensive overview, ensuring readers are informed about this condition, how it compares to other skin infections, and its treatment options.
Overview of Bacterial Skin Infections
Skin infections caused by bacteria can range from mild to severe, and erysipelas is one such infection that requires prompt medical attention. It typically presents as a raised, well-demarcated area of inflammation. While erysipelas is less common than conditions like impetigo or cellulitis, it is important to recognize its symptoms early to prevent complications. Timely intervention can help mitigate the discomfort and potential spread of the infection.
Causes of Erysipelas
Common Bacterial Causes
Erysipelas is predominantly caused by Group A Streptococcus, the same bacteria responsible for strep throat. This bacterium enters the skin through cuts, sores, or other breaks in the skin barrier. It is more common in individuals with compromised immune systems or pre-existing conditions like diabetes. Understanding the bacterial origin helps in tailoring effective antibiotic therapy.
Risk Factors for Developing Erysipelas
Several factors can increase the risk of developing erysipelas. These include chronic skin conditions like eczema or athlete's foot, a history of erysipelas or cellulitis, and conditions that cause swelling in the legs. People with lymphedema or those who are overweight may also be at increased risk. Awareness of these risk factors can aid in early identification and prevention.
Symptoms and Diagnosis
Recognizing the Symptoms of Erysipelas
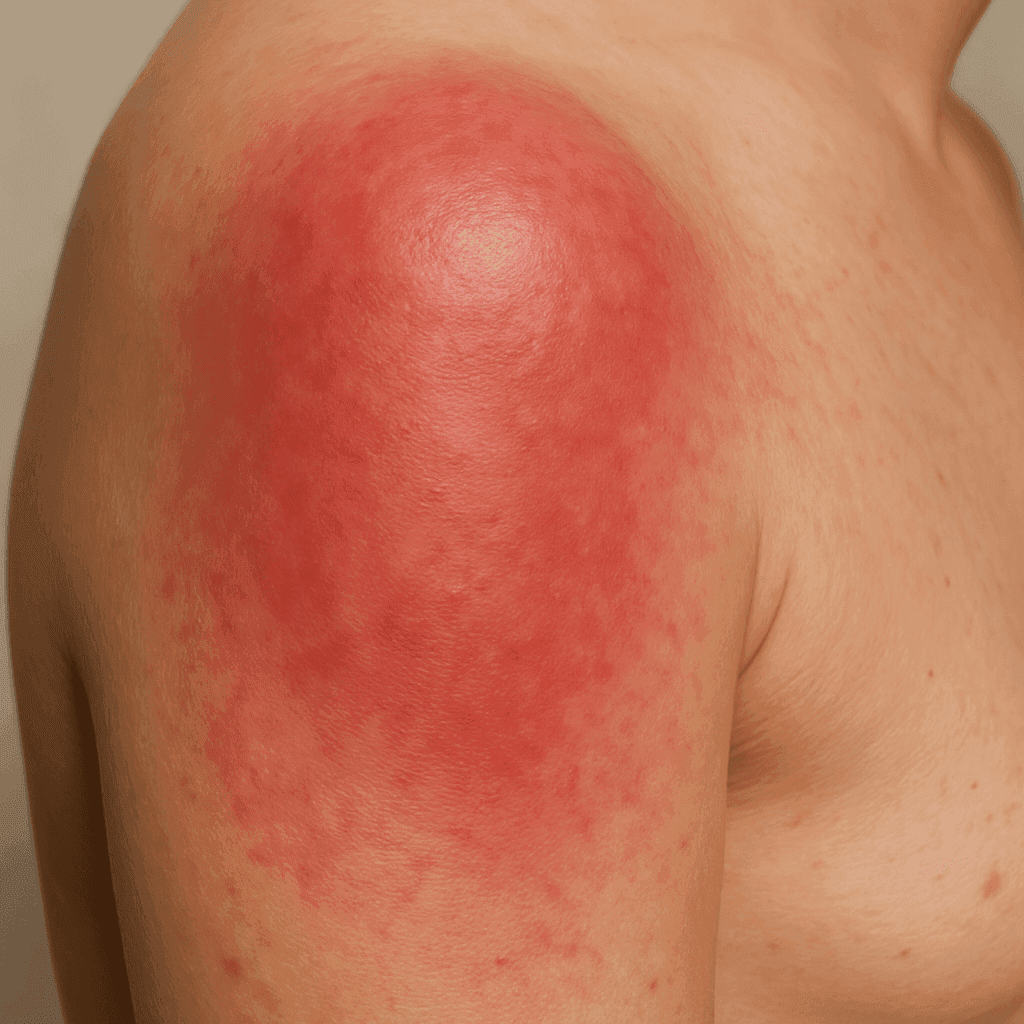
Symptoms of erysipelas include high fever, chills, and a red, swollen, and painful rash usually on the face or legs. The edges of the rash are typically raised and distinct. Other symptoms may include blisters on the affected area, swollen glands, and a general feeling of illness. Recognizing these symptoms early can prompt individuals to seek medical care before complications arise.
How Erysipelas is Diagnosed
Diagnosis of erysipelas is primarily clinical, based on the appearance of the rash and patient history. Physicians may perform a physical examination and inquire about recent injuries or infections. Blood tests and cultures can be used to confirm the diagnosis, although they are not always necessary. Accurate diagnosis ensures appropriate treatment and reduces the risk of recurrence.
Treatment Options
Antibiotic Treatments for Erysipelas
Antibiotics are the primary treatment for erysipelas, with penicillin being the most commonly prescribed. For those allergic to penicillin, alternative antibiotics like erythromycin or clindamycin may be used. Treatment usually lasts for about 7-14 days, depending on the severity of the infection. Adhering to the prescribed antibiotic regimen is crucial for complete recovery.
Home Care and Management
In addition to antibiotics, home care plays a vital role in managing erysipelas. Rest, elevating the affected limb, and applying cool compresses can help alleviate symptoms. Keeping the skin clean and moisturized can prevent further infection. Over-the-counter pain relievers may also be recommended to manage discomfort.
When to Seek Medical Attention
Immediate medical attention is necessary if symptoms do not improve within a few days of starting antibiotics, or if they worsen. Signs that require urgent care include increasing redness, high fever, or signs of infection spreading. Consulting a healthcare provider ensures appropriate intervention and prevents serious complications.
Erysipelas vs Other Skin Infections
Erysipelas vs Cellulitis
While erysipelas and cellulitis are similar, they differ in their depth and severity. Erysipelas affects the upper layers of the skin and has a well-defined border, whereas cellulitis extends deeper into the subcutaneous tissues and often has a more diffuse appearance. Understanding these distinctions is important for appropriate treatment and management.
Erysipelas vs Impetigo
Impetigo is a superficial skin infection, often seen in children, characterized by honey-colored crusts. Unlike erysipelas, impetigo is highly contagious. Both infections require antibiotic treatment, but the approach may vary based on the severity and specific organism involved.
Complications and Risk Management
Potential Complications of Erysipelas
If left untreated, erysipelas can lead to severe complications such as abscess formation, sepsis, or spread to deeper tissues. It can also result in recurring infections or chronic lymphedema. Early treatment and monitoring are essential to prevent these outcomes.
Preventing Recurrence of Erysipelas
Preventive measures include managing underlying conditions, maintaining good skin hygiene, and protecting the skin from injuries. Regular follow-ups with a healthcare provider can help monitor and manage any underlying risk factors. Education on recognizing early signs of infection aids in prompt treatment and prevention.
Erysipelas in Different Populations
Erysipelas in Children
Children can develop erysipelas, often after a minor injury or insect bite. Due to their developing immune systems, children may experience more pronounced symptoms. Pediatricians typically manage treatment, focusing on antibiotic therapy and supportive care.
Erysipelas in the Elderly
The elderly are at higher risk for erysipelas due to age-related skin changes and potential comorbidities. They may experience more severe symptoms and require hospitalization. Regular skin checks and preventive care are recommended to reduce the risk.
Special Considerations for Diabetics
Individuals with diabetes have an increased risk of skin infections like erysipelas due to compromised immune function and circulation issues. Blood sugar control and foot care are crucial in preventing infection. Diabetics should be vigilant about any skin changes and seek prompt medical attention if erysipelas is suspected.
FAQs about Erysipelas
- What is the main cause of erysipelas?
The main cause is infection by Group A Streptococcus bacteria. - How long does it take to recover from erysipelas?
Recovery typically takes 1-2 weeks with appropriate antibiotic treatment. - Can erysipelas be prevented?
Yes, through good skin care, managing underlying conditions, and preventing skin injuries. - Is erysipelas contagious?
Erysipelas itself is not highly contagious, but the bacteria causing it can spread through direct contact. - What should I do if I suspect I have erysipelas?
Seek medical attention promptly to receive appropriate diagnosis and treatment. - Can erysipelas lead to other health issues?
If untreated, it can cause serious complications like sepsis or chronic swelling.